8. Respiratory Disorders
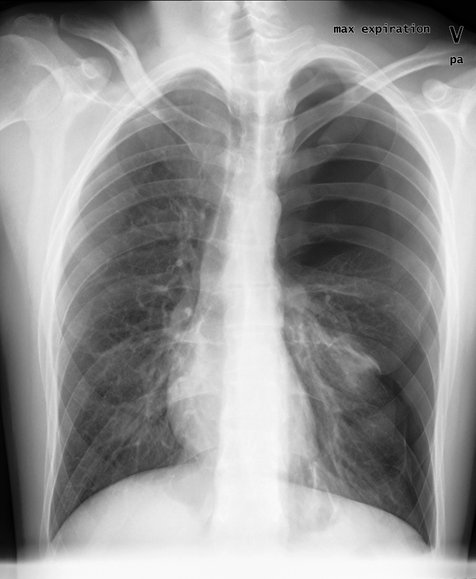
Pneumothorax on left side with onsetting tension pneumothorax. Must be treated before flying.
Photo:
Dept. of Radiology, Herlev Hospital.
General
Consider the following issues when a patient with a respiratory disorder is going to be repatriated:
Can the patient cope with the hypoxia experienced due to decreased oxygen tension at cruising altitude?
Is there any trapped air in the body’s cavities or other closed spaces that may aggravate any medical conditions (e.g. pain, circulatory, or respiratory) as the surrounding pressure changes during ascent or descent?
Pre-flight assessment
There is no single test that can predict whether a patient will desaturate during the next flight and that can be carried out in a general setting. A pre-flight assessment is made based on anamnesis and clinical evaluation. When performing a pre-flight evaluation, one or more of the following findings can be used:
• Previous air travel intolerance with significant respiratory symptoms.
• Walk tests (Self-Paced Walk Test usually 50 m (SPWT), Stair Climb Test (SCT), Six-Minute Walk Test
(6MWT), or Twelve-Minute Walk Test (12MWT)).
• SaO2 at sea level.
• ABG puncture.
• Pulmonary function tests (PFT), especially FEV1, FVC, and PEF.
• Blood samples (Hgb, in patients with cancer also K+, Na+, Ca++, Mg++).
• NYHA or CCS class.
• Hypoxic challenge testing (HCT).
Guidance for the interpretation of test results
Unescorted
Patients are usually accepted as unescorted passengers if:
• They can walk 50m or climb the stairs to the first floor at an acceptable pace.
• SaO2 > 94% at rest without auxiliary oxygen supply.
• SaO2 > 94% at rest with auxiliary oxygen supply, presuming that the condition is in a stable phase.
It is mandatory that the patient is confident with the use of oxygen therapy. If not, a trained
medical escort (e.g. a nurse) should accompany the patient. Flow rates should typically be
doubled during flight.
Escorted by physician
Patients escorted by a physician are usually accepted as passengers if:
• SaO2 < 94% at rest with auxiliary oxygen supply, presuming that the condition is in a stable phase.
• A patient with chronic lung insufficiency and who is partially bed-ridden and unable to walk
without dyspnoea may be transported in the sitting position with a small auxiliary oxygen supply, provided that a blood gas analysis shows normal pH irrespective of PaCO2 level, PaO2 > (6)-7 KPa, O2 saturation > 90% on atmospheric air, and provided that either the respiratory rate or the
patient’s dyspnoea are at their normal levels.
Patients who are considered unstable regarding respiratory function, or who are in a state of respiratory failure, or who do not fit any of the abovementioned categories, should be transported by air ambulance or PTCA.
Selected respiratory disorders with potential complications
when travelling by air
All patients should fulfil the abovementioned criteria in addition to those stated here.
Infectious diseases
Pneumonia
Patients with acute pneumonia or bronchitis are not accepted as passengers by commercial airlines. They are normally accepted on board when they are afebrile, in a normal respiratory state, and not contagious. (See also chapter 16).
Chronic respiratory problems
Asthma
The commercial flight environment does not usually pose problems for those with asthma.The main risk is bronchospasm induced by the low cabin humidity and the stress caused by travelling. Anamnestic information of previous air travel intolerance with significant respiratory symptoms is of utmost importance.
Patients with stable and well-controlled asthma can usually travel unescorted. Medication should be in the “carry on” luggage. All medications should be transported in their original, labelled containers along with documentation, e.g. a letter ("to whom it may concern”) from the treating physician or GP.
Unstable patients and patients that often have asthma attacks should be well controlled before travelling and escorted by a physician carrying the necessary equipment to intervene (drugs and oxygen).
Chronic Obstructive Pulmonary Disease (COPD)
Patients with acute exacerbations of COPD must return to a stable and well-controlled state before travelling. Please consult “Guidance for the interpretation of test results”.
Cystic fibrosis
The patient should be escorted by a physician with auxiliary oxygen supply if FEV1 < 50%.
Interstitial lung disease
Each case should be presented to the airline’s medical officer. Please note that this group of patients has an irreversible decrease in oxygen diffusion capacity and therefore reacts differently to hypoxia than other patients with respiratory diseases.
Obstructive Sleep Apnoea (OSAS) and Obesity Hypoventilation Syndrome (OHS)
Patients suffering from OSAS or OHS need a CPAP device during sleep. It is a machine that blows air through a hose to a mask that you take over your nose when you go to sleep. Of course, it presents challenges if you must use it during a flight. For these patients, it is therefore recommended that they, if possible, fly during the day and avoid sleeping during the flight. On longer flights where it is necessary to sleep and where they need to use their CPAP device, the following must be arranged:
- Book a seat in the plane where the patient can lie down, ie. in business class with reclining or full
flat seat.
- Airline approval for carriage and use of the CPAP device, including battery specification,
must be gained before travel.
- Permission to carry the CPAP device as hand luggage.
- Carry a hospital letter to advise that the patient need to use CPAP device during sleep.
Other problems in thorax and lungs
Pneumothorax
Untreated pneumothorax
Patients with a closed pneumothorax should not travel on commercial flights.
In very rare emergency cases, patients with closed pneumothorax may be evacuated to a hospital where the necessary medical expertise is present in order to treat the patient. In such cases, evacuation should be done with the cabin pressure at 1 atm (“sea-level flight”). The patient should be escorted by the “best available” medical personnel.
Treated pneumothorax where the chest tube is in situ
Most airlines will accept this type of patient if the lung is completely inflated without the use of active suction. The chest-tube must be connected to a Heimlich valve (one-way valve). The inflation of the lung must be documented with a chest x-ray taken shortly before the transportation. The patient must be escorted by a physician capable to perform a chest-tube insertion. The use of a water-seal type valve in a pressurized cabin is contra-indicated because of the risk of water being sucked into the pleural cavity.
Treated pneumothorax where the chest tube has been removed
Spontaneous pneumothorax should undergo definitive treatment to prevent recurrence before flying if possible. The patient will not be medically cleared by the airline before a chest x-ray, CT scan, or MRI scan taken at least 24 hours after the removal of the chest tube demonstrates a completely re-expanded lung.
The examinations must be repeated if a residual pneumothorax persists until complete re-expansion of the lung.
The rules of the airline companies
Patients treated for spontaneous pneumothorax may usually fly one to two weeks after the removal of the chest tube if fully recovered. Patients treated for traumatic pneumothorax may usually fly two weeks after the removal of the chest tube if fully recovered.
A few airlines will allow patients escorted by a physician to fly two days after the removal of the chest tube if a chest x-ray, CT scan, or MRI scan demonstrates a completely re-expanded lung.
The requirements regarding whether patients treated for pneumothorax can fly unaccompanied differs among airlines, so it is advisable to present patients with pneumothorax to the airline’s medical officer when ready for repatriation.
Rib and sternum fractures
Simple rib fractures do not normally give rise to aeromedical problems as long as the lung is undamaged and there is no pre-existing lung disorder. Generally, the principal problem associated with rib and sternum fractures is pain, which can lead to reduced respiration. It is therefore extremely important that the patient receive adequate treatment against pain.
Multiple rib fractures or double fractures can cause thoracic instability and respiratory insufficiency. These cases should be presented to the airline's medical officer.
Lung contusion
In the case of patients with acute respiratory insufficiency (shock lung, contusion), flying should be delayed until lung function has returned to normal. Should air transportation be unavoidable, an ambulance flight or PTC will often be required.
Subcutaneous emphysema
Patients who present subcutaneous emphysema may not be transported by commercial flight. If air evacuation is necessary, these patients may only be transported with a cabin pressure of 1 atm (“sea-level flight”).
Mediastinal emphysema
Patients presenting mediastinal emphysema may not be transported by commercial flight. If air evacuation is necessary, these patients may only be transported with a cabin pressure of 1 atm (“sea-level flight”).
These cases should be presented to the airline’s medical officer when ready for repatriation.
Heart transplantation (HTX) / Lung transplantation (LTX)
These cases should be presented to the airline’s medical officer when ready for repatriation.
Lung cancer
Chemotherapy, radiotherapy, or stent treatment should be presented to the airline’s medical officer. Since most of these modalities are intended as palliative treatment, the general condition of the patient may be poor. One should also consider the risk of, for example, metastasis, hydrothorax, or electrolyte derangement. (Please see Chapter 18).
Surgery
Lobectomy or pneumonectomy.
These cases should be presented to the airline’s medical officer when ready for repatriation. In cases with pneumonectomy, a chest x-ray, CT scan or MRI scan is essential to demonstrate that the potential pleural space is replaced by liquid and that there is no deviation of the mediastinum. The replacement of gas with fluid usually takes around six weeks.
Haemoptysis
Patients presenting with haemoptysis may not be transported by commercial flight until the cause is found and treated.
Hydrothorax and pleuracentesis
The patient should undergo diagnostic procedures before being presented to the airline’s medical officer. If pleuracentesis is performed, a chest x-ray, CT scan, or MRI scan taken at least 24 hours after the procedure must demonstrate the absence of pneumothorax.
001. Frontpage
001. Foreword
001. Contributors
001. Aeromedical Problems
012. Planning the Air Transportation of Patients
013. Airline Requirements
015. Transportation of Disabled Persons
016. Cardiac Disorders
019. Gastrointestinal Disorders
010. Central Nervous System Disorders
011. Ear, Nose, and Throat Disorders
012. Eye Disorders
013. Mental Disorders
014. Gynaecological and Pregnancy Problems
015. Transportation of Sick Children
016. Infectious Diseases
017. Orthopaedic Injuries
018. Cancer
120. Acute Mountain and Decompression Sickness
021. Burns and Plastic Surgical Problems
122. Airsickness
123. Jet Lag
124. The STEP System
125. Specialised Transportation of Patients
126. First Aid on Board – Legal Considerations
27. The History of Air Transportation of Patients
28. Oxygen supplementation in flight - a summary
Latest update: 19 - 09 - 2022